Alcohol and the Heart: Fact vs. Fiction
- Mar 30
- 15 min read
Updated: Apr 17

Key Takeaways
|
Table of Contents |
Why Alcohol Is Different From Other Substances
One of the more challenging discussions a patient faces when talking to their doctor is the conversation about the patient’s alcohol intake. The patient who smokes cigarettes or uses illicit substances such as heroin is more likely to accept that they are doing something potentially harmful to their bodies, so the tone of the discussion around these substances has less friction. However, alcohol consumption is normalized and encouraged directly in our media and associated marketing, so people may be less likely to think they need to monitor their alcohol consumption and may be less interested in hearing criticisms of their alcohol intake. Annual advertising spend across all media in the United States over the last few years suggested that $8B was spent for alcohol, $8B for tobacco, and $10B was spent by pharmaceutical companies. Consequently, substantial amounts are being spent to influence our behaviors and potentially normalize them.
Who Uses Alcohol — and Why
Unfortunately, while many find the effects of alcohol to be a pleasant distraction and an important part of socialization, many people use alcohol as a treatment for a variety of conditions such as anxiety, depression, sleep disorder, and chronic pain (Crum, 2013; Ferguson 2023). Nearly one quarter of those patients with mood disorders self-report using alcohol to treat their symptoms (Crum, 2013). A recent study by Krist and Bradley (2025) suggested that 10% of Americans have an alcohol use disorder and 20-30% of patients in outpatient medical settings have unhealthy alcohol use. Unfortunately, only 20% of people with an alcohol use disorder seek treatment for their alcohol use behavior (Grant, 2015).
What Counts as a Standard Drink?
Part of the problem in discussing alcohol use can be uncertainty in the discussion around what a standard drink is and how much alcohol intake is too much. As shown in Figure 1, adapted from NIH and Dietary Guidelines, there is a wide variation of alcohol amount by volume in terms of what constitutes “a drink.” While people will frequently disagree on how much alcohol intake is “normal”, it becomes safer to try to define what is “abnormal”, though even that is challenging.

Figure 1. Standard drink, adapted from NIH and DietaryGuidelines.gov
Women: ≥4 drinks per day or ≥8 drinks per week
Men: ≥5 drinks per day or ≥15 drinks per week
The fact that there are different cutoffs between men and women can raise some concern among patients, but there is a biological basis. Compared to men, women generally:
Absorb more alcohol than men
Have less alcohol processing activity in their stomach
Take longer to process the same amount of alcohol due to lower overall amounts of alcohol dehydrogenase enzymes in their bodies
The result of these gender-based differences is that women can achieve higher blood alcohol concentrations than men even after consuming similar amounts of alcohol.
Alcohol and the Heart
By this point, you may be thinking, “Ok, we know too much alcohol can be bad, but why does this matter to a cardiologist?” An excellent resource discussing alcohol and its cardiovascular impacts was released in 2025 by Piano et al. In that article, the World Health Organization is cited as indicating consuming any amounts of alcohol has health risks and the Canadian guidelines indicates that drinking less is better. The American dietary guidelines previously had set limits on alcohol intake, yet the most recent version of the guidelines removed those guardrails, essentially only suggesting vague moderation. One has to wonder if the removal of the guidance on limiting alcohol intake wasn’t influenced by those groups who would benefit from increased alcohol sales (Brems, 2023; Moynihan, 2020).
Most people will have some sense that there can be harmful effects related to alcohol intake, though they may think more of the person who makes creative choices while under the influence of alcohol – the “hold my beer” moments – and gets hurt. Certainly, a very concerning related issue is those who are hurt, or hurt others, while operating motor vehicles under the influence of alcohol. However, the focus on this piece is to address the harms of alcohol to our bodies, particularly the heart.
It is important to note that any type of alcohol can cause alcohol-related heart problems. It’s not only hard liquor that can damage the heart, but also wine and beer. I have unfortunately had too many encounters where I told a patient they had an alcohol-related cardiomyopathy or systolic heart failure, but they indicated they only drank beer and they didn’t think beer could be bad for them. Too many times I have heard, “I don’t drink alcohol. I just drink beer.”
Before delving into the specifics of harm, it remains important to address that earlier studies may have yielded conflicting results due to self-reported data, which becomes less reliable with higher consumption levels. Also, early studies were inconsistent in terms of alcohol doses, such as which alcohol form (e.g., beer vs. wine) was consumed and how much. More recent trials attempt to improve the self-reporting of data (e.g., smartphone apps to log consumption), smart devices to monitor blood alcohol with transdermal sensors, and home urine kits for alcohol consumption monitoring (Piano, 2025). This isn’t to say earlier results are to be discarded, but it may explain some variation of earlier trials.
There are at least five different types of heart and heart-related complications related to alcohol consumption (Piano, 2025). They include:
Cardiomyopathy and Heart Failure
Arrhythmia or Abnormal Heart Rhythms
Blood Pressure
Stroke
Coronary Artery Disease and Heart Attacks
Cardiomyopathy and Heart Failure
Alcohol can directly damage heart muscle and lead to at least two kinds of heart muscle damage. At lower alcohol intake levels, alcohol can be associated with a stiffening of the heart muscle. This stiffening can be referred to as diastolic dysfunction or diastolic heart failure. A stiff heart may be strong, but inflexible. To get a sense of what diastolic dysfunction is, picture the weight lifter that has massive muscles, but may not be able to reach their toes. The person is strong, but inflexible. When people have diastolic dysfunction, they may get hospitalized with heart failure due to the body accumulating too much fluid, particularly in the lung tissue, and the person becoming short of breath. Low alcohol intake levels, even just four drinks in a week, can be associated with worsening diastolic dysfunction.
The other main type of heart failure, distinct from diastolic dysfunction, is systolic dysfunction or systolic heart failure. With this type of heart failure, the heart muscle is so damaged by the chronic alcohol intake that the heart weakens and may dilate. In this person, hospitalization from heart failure is also related to fluid in the lungs and shortness of breath. However, with systolic heart failure, fluid builds up because the heart is too weak to push the blood forward, while with diastolic heart failure, fluid builds up because the heart cannot relax quickly enough to accept the next load of blood entering the heart.
Dysfunction vs. Heart Failure
A person may have systolic/diastolic dysfunction, but if they are not having symptoms they may not be having systolic/diastolic heart failure. |
Alcohol-related cardiomyopathy (ARC) accounts for nearly 1 in 1,000 hospitalizations, affecting men slightly more often than women, and with an average age in the mid-50’s. Men are thought to develop ARC with at least seven drinks per day in as little as five years, while women may develop ARC with a lower alcohol dose. Once people consume over 21 drinks per week, their risk of ARC increases significantly. The risk of developing ARC with two or fewer drinks per day is less clear.
A bit of a silver lining in the discussion is that those people who abstain from alcohol after being defined as having systolic heart failure (recall this is the group with the weak pump) may have substantially improved heart function in 2-3 years after diagnosis, so long as they abstain from alcohol (Lupon, 2018). The Lupon study has important caveats, though, in that participants were 77% male and 99% white, so the broad applicability is limited. Nonetheless, other publications also highlight the importance of abstinence being mandated for the best chances of full recovery (Bozkurt, 2016). Interestingly, the Bozkurt piece highlights the importance of considering thiamine (vitamin B1) and folate (vitamin B9) supplements in those with alcohol cardiomyopathy if they have low serum levels as those deficiencies may be seen more frequently in those with higher levels of alcohol consumption and thiamine deficiency can worsen cardiomyopathy.
Arrhythmia
There are a number of arrhythmias commonly seen in cardiology, including supraventricular tachycardia (SVT), ventricular tachycardia (VT), and ventricular fibrillation (VF). People may also feel sensations of “extra beats” or palpitations related to premature ventricular contractions (PVC). Alcohol does not appear to worsen SVT, PVC’s, VT, or VF. However, while no clear signals are noted with worsening VT/VF, alcohol is associated with sudden death (Piano, 2025; Voskoboinik, 2016).
In contrast, alcohol has a reproducible causal effect on atrial fibrillation and may also worsen atrial flutter (Piano, 2025). Those women who drink 2 or more drinks routinely are 60% more likely to develop atrial fibrillation (Conen, 2008). Each drink carries added risk, with each drink consumed daily adding 8% risk of atrial fibrillation, with increased risk seen even among those with low alcohol consumption (Larsson, 2014). Stopping alcohol consumption completely will decrease the chance that atrial fibrillation will recur. Conversely, there is a strong association where alcohol can trigger atrial fibrillation episodes.
The combination of worsening atrial arrhythmias and sudden death associated with binge drinking has been labeled “holiday heart.” It is not uncommon to see a surge in hospitalizations for heart failure and atrial fibrillation associated with binge consumptions around holidays such as New Year’s Eve and Thanksgiving. Evidence that “holiday heart” can be seen outside of national holidays can be seen in Wisconsin, where the opening weekend of gun deer season is also associated with increased “holiday heart”, presumably due to the increased alcohol consumption related to hunting traditions.
Blood Pressure
The messaging around the impact of alcohol on blood pressure can be confusing. Some pieces suggest that lower alcohol consumption may not lead to lasting impacts on blood pressure (Piano, 2025). However, more often, consensus documents favor abstinence instead of tolerance of even low-level alcohol intake (Jones, 2025).
Stroke
Consuming at least two drinks per day is associated with increased risk of stroke, particularly if the person consumes at least four drinks per day (Piano, 2025; Smyth, 2023). The influence of consuming fewer than two drinks per day on stroke incidence is less clear. Importantly, as alcohol substantially increases the risk of atrial fibrillation and atrial fibrillation increases the risk of stroke, it is important to understand if the stroke risk is directly due to alcohol or if the stroke risk is driven by the presence of atrial fibrillation.
Coronary Artery Disease
Heavy or binge alcohol consumption is associated with a significant increase in the risk of coronary artery disease (CAD) and heart attack (Piano, 2025). While some articles implied a possible benefit for lower levels of alcohol consumption, this claim is refuted by other articles (Biddinger, 2022; Hu, 2022; Rosoff, 2020).
Epigenetics and Alcohol
Epigenetics involves changes not to a person’s DNA itself, but to the structure around the DNA which impacts how the DNA is actually utilized. These epigenetic changes include DNA methylation, histone modification, and also impacts on RNA (Wu, 2021). The epigenetic changes driven by chronic alcohol consumption have been suggested to play a significant role in people developing alcohol-related cardiomyopathy. Importantly, it appears abstaining from alcohol may provide some degree of reversal of alcohol’s epigenetic changes to the heart and may suggest a potential mechanism for why abstinence is needed for the highest odds of recovery. This potential for epigenetic reversal with abstinence may, in fact, help explain the recovery of heart function observed in the Lupon (2018) study, where patients with alcohol-related systolic heart failure who abstained saw substantial improvement in their ejection fraction over just two to three years.
Young Adults
Binge alcohol consumption, particularly in those 18-30 years old, is associated with endothelial dysfunction, coronary artery calcification, and stiffening of the arteries. Consequently, binge alcohol consumption may be seen as a significant contributing factor to premature coronary disease. Furthermore, binge alcohol consumption in young adults is also associated with a substantial increase in the risk of ischemic stroke, potentially related to the same vascular changes.
Regional Differences
I have lived and practiced medicine in Wisconsin for nearly the same duration I lived and practiced outside of Wisconsin. The regional differences in local opinions of what is normal or acceptable alcohol consumption has been striking. And it’s not only my impression. Wisconsin has repeatedly been found to have well above average alcohol consumption, whether it is per person or measures of binge drinking. At the per person level, Wisconsin was #8 at 2.93 gallons per year, but was #2 in terms of excessive drinking at 24.5%. Of the 49 states surveyed, Wisconsin was 4th worst with over 20% of those who consume alcohol indicating they binge drink. In another reference, Wisconsin was the only state in the country where every county in the state had high excessive drinking (Figure 2). Taken together, alcohol is a prominent part of Wisconsin life and should be part of healthcare discussions to bring awareness to what “healthy” alcohol consumption may look like, though the data suggest there may not be a truly “healthy” amount.

Can Alcohol be “Healthy”?
One of the more common issues that comes up with those who drink alcohol is that they aren't aware of how many calories are in each drink. The context for these discussions is that a healthy diet and weight form the core of overall cardiovascular health. Few would argue that drinking too many sugary sodas or juices could create a problem. However, people frequently don't consider their alcohol intake when counting calories. As shown in Figure 3, alcohol containing beverages contain a real amount of calories, which is particularly important when you think about how many people don't stop at just one drink in a night.
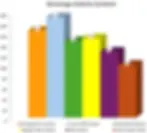
Figure 3. Calorie content of typical beverages
In addition to considering the total calories consumed when deciding on how healthy alcohol is, a more important issue is the fact that alcohol is a carcinogen in the same class as tobacco and asbestos. It is estimated that 1 in 6 cases (16%) of breast cancer in women, 1 in 4-5 (23%) cases of liver in men, and 1 in 25 (4%) cancers of all types worldwide are due to alcohol (Gapstur, 2023). Given the multiple negative impacts on the heart and the increased risk of cancers due to alcohol, it remains challenging to suggest there can be a healthy alcohol intake level.
Even when setting aside the carcinogenic potential of alcohol, there have been publications intimating that low levels of alcohol may be healthy, both in the lay press and scientific publications (Tu, 2021). When risk from an event, such as a heart attack, goes down initially but then rises above baseline with higher intake, that is called a J-shaped curve. A common reference with alcohol is that low-moderate intake may be associated with a J-shaped curve in terms of cardiovascular measures, as suggested with a low-level intake of alcohol and risk of atrial fibrillation (Tu, 2021). A simulated J-shape curve is shown in Figure 4. However, an important evaluation with a thorough evaluation of comorbidities found that the J-shaped curve was removed when correcting for healthy lifestyle habits (Biddinger, 2022). They suggested that those who stopped drinking after only one drink may be making other, healthier choices that were contributing to better cardiovascular outcomes and not actually that the alcohol was providing a health benefit. Also, the resveratrol content of red wine that was initially promoted was later not felt to have been important for cardiovascular disease (Forman, 2023).

Figure 4. Simulated J-Shape curve depicting reduced risk of a sample outcome with low level alcohol intake, but increased risk with higher alcohol intake.
Alcohol Makes Other Chronic Conditions Harder to Manage
An important issue that may not at first be obvious is that those with other chronic conditions aside from alcohol-related effects on the heart is that those with heavy or binge alcohol consumption may have worse outcomes from non-cardiac conditions (Piano, 2025). With binge alcohol consumption, patients may be more inclined to neglect medicines and other care related to the other conditions such as high blood pressure and diabetes, potentially worsening their outcomes (Bryson, 2008).
Summary
Taken together, we have substantial data supporting the harm of even modest alcohol consumption, particularly with respect to atrial arrhythmia and heart failure. The primary European and American Cardiology societies share a similar position that no amount of alcohol consumption should be consumed to specifically improve cardiovascular health (Fegers, 2022).
Guidelines are clear to state that nondrinkers should not be advised to start drinking to improve cardiovascular health. An attempt to understand the role of alcohol and cardiovascular health was a study called the Moderate Alcohol and Cardiovascular Health (MACH15) trial, but it was halted by the American National Institutes of Health due to concerns of excessive industry involvement (Mitchell, 2020). A new attempt at studying moderate alcohol consumption is being undertaken in Spain, funded by the European Research Council and called the University of Navarra Alumni Trialist Initiative (UNATI). UNATI is scheduled to run from 2023 to 2029. This trial aims to understand the impact of moderate alcohol consumption on a variety of health issues including cardiovascular disease, diabetes, liver disease, and dementia by having half of the 10,000-person study group stop drinking any alcohol for five years.
People who have concerns about their alcohol intake should discuss it with their doctor, particularly if they have any of the heart-related concerns above. Symptoms to be aware of that may be a sign of heart-related involvement from alcohol excess include unexplained shortness of breath or inappropriately racing heartbeat. It is encouraging that much of the harms of alcohol can improve with abstinence from alcohol.
References:
Biddinger, K.J., et al. Association of Habitual Alcohol Intake With Risk of Cardiovascular Disease. JAMA Network Open. 2022;5(3):e223849
Bozkurt, B., et al. Current Diagnostic and Treatment Strategies for Specific Dilated Cardiomyopathies. Circulation. 2016; 134:e579
Brems, J.H., et al. Intellectual conflicts of interest among cardiology and pulmonology clinical practice guidelines. PLOS One. 2023; 18(7):e0288349
Bryson, C.L., et al. Alcohol screening scores and medication nonadherence. Annals of Internal Medicine. 2008; 149(11):795
Conen, D., et al. Alcohol Consumption and Risk of Incident Atrial Fibrillation in Women. JAMA. 2008; 300(21):2489
Crum, R.M., et al. A Prospective Assessment of Reports of Drinking to Self-medicate Mood Symptoms With the Incidence and Persistence of Alcohol Dependence. JAMA Psychiatry. 2013; 70(7):718
Fegers-Wustrow, I., et al. Comparison of American and European Guidelines for Primary Prevention of Cardiovascular Disease. Journal of the American College of Cardiology. 2022; 79(13):1304
Ferguson, E., et al. Association of therapeutic and recreational reasons for alcohol use with alcohol demand. Alcohol. 2023; 31(1):106
Forman, D.E., et al. Impact of Geroscience on Therapeutic Strategies for Older Adults With Cardiovascular Disease. Journal of the American College of Cardiology. 2023; 82(7):631
Gapstur, S.M., et al. The IARC Perspective on Alcohol Reduction or Cessation and Cancer Risk. The New England Journal of Medicine. 2023; 389(26):2486
Grant, B.F., et al. Epidemiology of DSM-5 Alcohol Use Disorder. JAMA Psychiatry. 2015; 72(8):757
Hu, C., et al. Causal associations of alcohol consumption with cardiovascular diseases and all-cause mortality among Chinese males. American Journal of Clinical Nutrition. 2022; 116(3):771
Jones, D.W. et al. 2025 AHA/ACC/AANP/AAPA/ABC/ACCP/ACPM/AGS/AMA/ASPC/NMA/PCNA/SGIM Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults. Journal of the American College of Cardiology. 2025; 86(18):1567
Krist, A.H., et al. Addressing Alcohol Use. The New England Journal of Medicine. 2025; 392:1721
Larsson, S.C., et al. Alcohol Consumption and Risk of Atrial Fibrillation. Journal of the American College of Cardiology. 2014; 64(3):281
Lupon, J., et al. Dynamic Trajectories of Left Ventricular Ejection Fraction in Heart Failure. Journal of the American College of Cardiology. 2018; 72(6):591
Mitchell, G., et al. Alcohol Industry Involvement in the Moderate Alcohol and Cardiovascular Health Trial. American Journal of Public Health. 2020; 110(4):485
Moynihan, R., et al. Financial ties between leaders of influential US professional medical associations and industry: cross sectional study. British Medical Journal. 2020; 369:m1505
Piano, M.R., et al. Alcohol Use and Cardiovascular Disease: A Scientific Statement From the American Heart Association. 2025; 152:e7
Rosoff, D.B., et al. Evaluating the relationship between alcohol consumption, tobacco use, and cardiovascular disease: A multivariable Mendelian randomization study. PLOS Medicine. 2020; 17(12):e1003410
Smyth, A., et al. Alcohol Intake as a Risk Factor for Acute Stroke. Neurology. 2023; 100:e142
Tu, S.J., et al. Risk Thresholds for Total and Beverage-Specific Alcohol Consumption and Incident Atrial Fibrillation. JACC Clinical Electrophysiology. 2021; 7(12):1561
Voskoboinik, A., et al. Alcohol and Atrial Fibrillation: A Sobering Review. Journal of the American College of Cardiology. 2016; 68(23):2567
Wu, L., et al. Epigenetic modification in alcohol use disorder and alcoholic cardiomyopathy: From pathophysiology to therapeutic opportunities. Metabolism. 2021; 125:154909
This post is for educational purposes only and does not constitute medical advice. Please consult a qualified healthcare provider for personalized guidance.
© Evexeya Health | Madison, WI | evexeyahealth.com
